Yes, GERD (gastroesophageal reflux disease) can cause shortness of breath, and it often shows up alongside other uncomfortable symptoms. Stomach acid flowing back into the esophagus can irritate the throat, airways, and even the lungs, leading to symptoms such as coughing, wheezing, chest tightness, or a sensation of not getting enough air. Some people notice these symptoms mostly at night or after large meals, while others experience them after consuming trigger foods like spicy dishes, fatty meals, caffeine, or chocolate.
Shortness of breath caused by GERD can feel sudden or persistent, making it easy to confuse with asthma, allergies, or even heart problems. This combination of symptoms, triggers, and urgency can leave readers curious to understand why their breathing is affected, when to take action, and how to prevent future episodes. When symptoms feel severe, seeking care at an ER in Pearland can help rule out serious conditions.
What Is GERD?
GERD is a chronic digestive disorder in which stomach acid frequently flows back into the esophagus. Normally, a muscle called the lower esophageal sphincter (LES) acts as a valve to prevent acid from moving upward. When this muscle weakens or relaxes at the wrong time, acid reflux occurs. While occasional reflux is common and usually harmless, GERD is diagnosed when this happens repeatedly and causes persistent symptoms or complications. Over time, constant exposure to stomach acid can damage the esophageal lining and affect nearby structures, including the respiratory system.
GERD can develop due to several factors, such as obesity, certain foods, smoking, pregnancy, or a hiatal hernia. If left unmanaged, it can lead to more serious health concerns, making early recognition and treatment important to prevent long-term complications.
Difference Between GERD and Acid Reflux?
Understanding the distinction between acid reflux and GERD is important because it helps determine when lifestyle changes are enough and when medical treatment is needed.
- Acid Reflux: Occasional backward flow of stomach acid into the esophagus, often triggered by heavy meals, spicy or fatty foods, or lying down too soon after eating. These episodes are usually temporary and manageable.
- GERD: A chronic and more severe condition with frequent acid reflux that disrupts daily life, causes discomfort, and may lead to complications. It typically requires long-term management, including lifestyle changes and sometimes medication.
Recognizing the difference ensures proper management and prevents long-term complications.
How Does GERD Cause Shortness of Breath?
GERD can affect breathing through several complex mechanisms. These go beyond simple acid irritation and involve interactions between the digestive and respiratory systems.
Airway Irritation and Inflammation
When acid travels up the esophagus, it can reach the throat and voice box. This area is closely connected to the airways, so irritation here can lead to inflammation. As a result, the airways may become sensitive or slightly swollen, making breathing feel restricted.
Micro-Aspiration into the Lungs
In some cases, tiny droplets of stomach acid can enter the lungs. This is called micro-aspiration. Even small amounts can irritate lung tissue, leading to symptoms such as coughing, wheezing, and shortness of breath. This is more likely to happen during sleep when the body is lying flat.
Vagus Nerve Response
The esophagus and lungs share a nerve called the vagus nerve. When acid irritates the esophagus, it can stimulate this nerve and trigger a reflex that tightens the airways. This can cause a sudden feeling of breathlessness, even without significant acid reaching the lungs.
Bronchospasm
GERD can also cause bronchospasm, a condition in which the muscles around the airways tighten. This narrows the airways and makes it harder to breathe. The sensation can be similar to asthma, and in some cases, GERD can worsen existing asthma symptoms.
Pressure After Eating
After large meals, the stomach expands and increases pressure on the diaphragm. This pressure can push acid upward and simultaneously make breathing feel more difficult. This is why symptoms often worsen after eating or when lying down.
Because of these factors, GERD-related shortness of breath is often more noticeable at night or after meals, and it may improve when sitting upright. However, if symptoms become severe or sudden, seeking an ER near you can help ensure prompt medical evaluation and care.
Symptoms That Shouldn’t Be Ignored
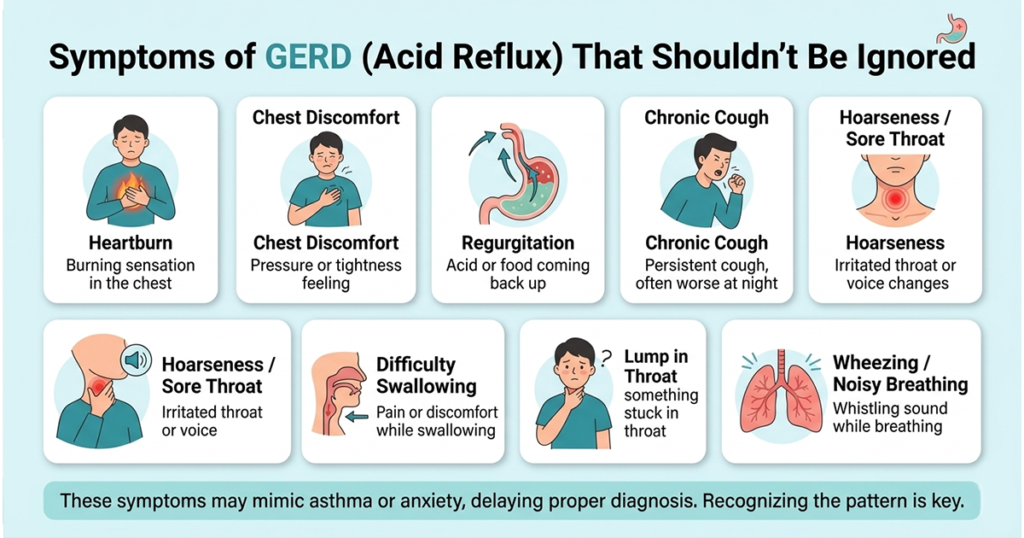
Shortness of breath caused by GERD usually appears alongside other digestive and respiratory symptoms. Recognizing this pattern is important for identifying the condition.
Common associated symptoms include:
- Persistent heartburn
- Chest discomfort or tightness
- Regurgitation of food or sour liquid
- Chronic cough, especially at night
- Hoarseness or a sore throat
- Difficulty swallowing
- A sensation of a lump in the throat
- Wheezing or noisy breathing
These symptoms may vary in intensity and frequency. In many cases, breathing issues are mistaken for asthma or anxiety, which can delay proper diagnosis.
How Is GERD Diagnosed?
Diagnosing GERD involves evaluating symptoms and, when necessary, conducting medical tests to confirm the condition.
- Medical History and Symptom Assessment: Doctors begin by reviewing your symptoms, lifestyle, and medical history. Frequent heartburn and reflux symptoms are strong indicators of GERD.
- Upper Endoscopy: This procedure uses a thin, flexible tube with a camera to examine the esophagus. It helps detect inflammation, damage, or complications such as ulcers.
- pH Monitoring: This test measures acid levels in the esophagus over 24 hours. It is one of the most accurate ways to confirm GERD.
- Esophageal Manometry: This test evaluates how well the esophagus and LES function. It helps identify muscle-related issues that may contribute to reflux.
- Additional Tests: In some cases, imaging or breathing tests may be used to rule out other causes of shortness of breath.
A proper diagnosis ensures that symptoms are not mistaken for more serious conditions such as heart disease or chronic lung disorders.
When GERD Becomes a Problem
GERD becomes a significant concern when symptoms are frequent, severe, or begin to interfere with daily life. You should pay attention if symptoms occur multiple times a week, shortness of breath becomes persistent, sleep is disrupted due to reflux, swallowing becomes difficult or painful, over-the-counter medications no longer provide relief, or there is unexplained weight loss or an ongoing cough. If left untreated, GERD can lead to complications such as esophagitis, strictures (narrowing of the esophagus), or Barrett’s esophagus, a condition that increases the risk of esophageal cancer. Early management can prevent these complications and improve overall quality of life.
Treatment Options
Managing GERD effectively usually requires a combination of lifestyle adjustments, dietary changes, and medical treatments. The goal is to reduce acid reflux, relieve symptoms, and prevent long-term complications.
Lifestyle Changes
Simple daily habits can significantly reduce GERD symptoms:
- Eat smaller, more frequent meals.
- Avoid trigger foods such as spicy, fatty, or acidic items.
- Maintain a healthy weight.
- Quit smoking and limit alcohol intake.
- Avoid lying down immediately after eating.
- Elevate the head of the bed by 6–8 inches to prevent nighttime reflux.
Medications
- Antacids: Provide fast, temporary relief by neutralizing stomach acid; ideal for occasional symptoms.
- H2 Blockers: Reduce acid production and offer longer-lasting relief than antacids, helping prevent reflux episodes.
- Proton Pump Inhibitors (PPIs): Stronger medications that significantly reduce acid production and allow the esophagus to heal; prescribed for moderate to severe GERD.
- Prokinetic Agents: Improve stomach emptying and strengthen the lower esophageal sphincter (LES), reducing the frequency of acid reflux.
Surgical and Procedural Options
For severe cases where medications and lifestyle changes are insufficient:
- Fundoplication: A surgical procedure that strengthens the LES to prevent acid reflux.
- Endoscopic Procedures: Minimally invasive techniques that improve LES function and reduce reflux episodes.
What Foods Are Good for GERD?
Diet plays a crucial role in managing GERD symptoms and preventing flare-ups.
Recommended Foods
- Whole grains such as oatmeal and brown rice
- Lean proteins like chicken, turkey, and fish
- Non-citrus fruits such as bananas and melons
- Vegetables, including leafy greens, broccoli, and carrots
- Low-fat or non-fat dairy products
- Herbal teas and natural remedies like ginger
Foods to Avoid
- Spicy and fried foods
- Fatty or greasy meals
- Citrus fruits and juices
- Chocolate and caffeine
- Carbonated beverages
- Tomato-based products
In addition to choosing the right foods, eating smaller portions and avoiding late-night meals can significantly reduce symptoms.
When to Go to the ER?
Although GERD is usually not life-threatening, certain symptoms require immediate medical attention.
Go to the emergency room if you experience:
- Severe or sudden shortness of breath
- Chest pain that spreads to the arm, neck, or jaw
- Difficulty breathing that worsens quickly
- Dizziness, confusion, or fainting
- Vomiting blood or passing black stools
These symptoms may indicate a more serious condition, such as a heart attack or severe gastrointestinal issue, and should never be ignored.
Expert Care for GERD-Related Shortness of Breath
Living with GERD that affects your breathing can be unsettling and exhausting. At Texas Emergency Care Center, our team provides attentive, expert care, focusing on identifying the root cause and offering targeted treatment to relieve symptoms like shortness of breath, chest tightness, and persistent coughing. With our support, you can breathe more easily and regain comfort in your daily life.
If symptoms worsen after meals, at night, or interfere with daily activities, prompt evaluation is crucial. Our compassionate professionals ensure timely assessment, effective treatment, and guidance to help you manage GERD safely, preventing complications and improving your overall well-being.
Key Takeaways
- GERD can cause shortness of breath through airway irritation and nerve reflexes.
- Symptoms often include heartburn, cough, and chest tightness.
- Breathing difficulties may worsen after eating or when lying down.
- Diagnosis involves evaluating symptoms and administering specialized tests.
- Treatment typically includes lifestyle modifications, medication, and dietary adjustments.
- Severe symptoms require immediate medical attention.
Frequently Asked Questions
How do I know if I have GERD?
Frequent heartburn, acid regurgitation, chest discomfort, or shortness of breath after meals may suggest GERD. Symptoms often worsen when lying down or after eating. A doctor can confirm the diagnosis through evaluation and testing.
What does GERD feel like?
GERD commonly causes a burning sensation in the chest (heartburn), a sour or acidic taste in the mouth, and discomfort after meals. Some people may also feel throat tightness or difficulty swallowing. Symptoms can vary in intensity.
How long does GERD last?
GERD is often a chronic condition that can last for weeks, months, or longer if untreated. Symptoms may come and go, but can persist without proper management. With treatment, flare-ups can be controlled effectively.