Acid reflux is a common digestive condition that occurs when stomach acid flows backward into the esophagus, the tube connecting the throat to the stomach. This happens when the lower esophageal sphincter (LES), a ring-shaped muscle that normally prevents stomach contents from moving upward, becomes weak or relaxes inappropriately. When acid enters the esophagus, it can irritate the lining and cause discomfort, including heartburn, chest pressure, nausea, or a sour taste in the mouth. Occasional reflux often happens after large meals or trigger foods and is generally mild.
However, frequent or persistent episodes may signal gastroesophageal reflux disease (GERD), a chronic condition that can damage the esophagus if untreated. Recognizing the signs of acid reflux early allows individuals to manage symptoms effectively. Timely medical care is important for preventing complications and improving digestive health.For professional evaluation and treatment, consulting an ER in Pearland specialist can help ensure proper management and relief.
How Acid Reflux Develops in the Body
The LES normally opens to allow food into the stomach and closes to prevent stomach contents from moving backward. When this valve becomes weak, stomach acid can flow upward into the esophagus.
- Esophageal Irritation: Repeated exposure to acid irritates and inflames the esophagus lining, causing discomfort.
- Inflammation and Esophagitis: Chronic reflux can lead to esophagitis, which may result in ulcers or scarring over time.
- Barrett’s Esophagus: Persistent acid exposure may change the cells lining the esophagus, increasing the risk of precancerous conditions.
- Impact on Sleep: Nighttime reflux can disrupt sleep due to discomfort or coughing.
- Respiratory Symptoms: Acid reaching the throat may trigger hoarseness, chronic cough, or asthma-like symptoms.
Common Symptoms of Acid Reflux
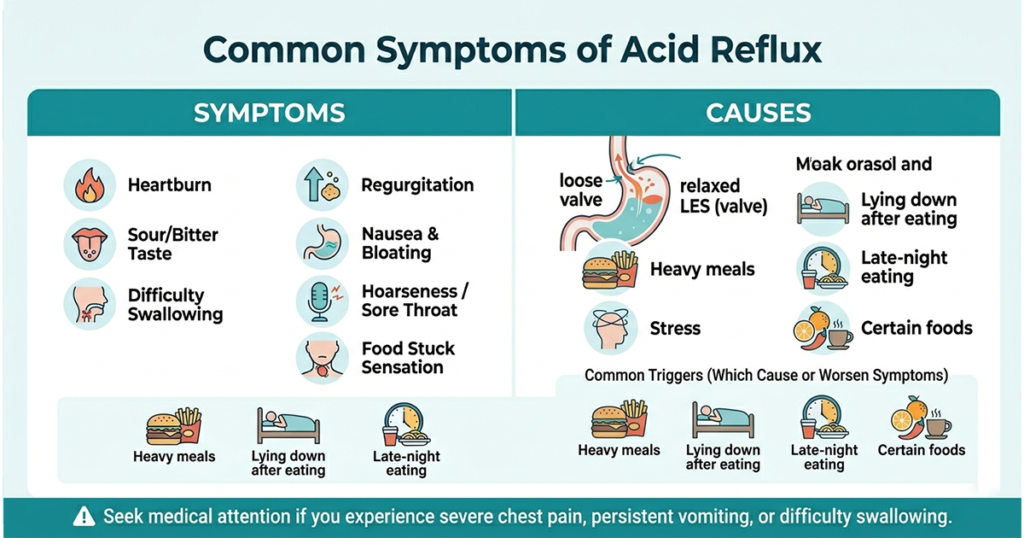
Acid reflux manifests in a variety of ways, from mild irritation to more severe discomfort.
- Heartburn: Burning sensation in the chest, often after meals or when lying down.
- Regurgitation: Backflow of stomach acid or undigested food into the mouth or throat.
- Sour or Bitter Taste: Acid moving upward may cause a noticeable taste in the mouth.
- Nausea and Bloating: Slower digestion can make you feel bloated, full, or nauseated.
- Difficulty Swallowing (Dysphagia): Inflammation can make swallowing uncomfortable or painful.
- Hoarseness or Sore Throat: Chronic reflux may irritate vocal cords and throat tissue.
- Feeling of Food Stuck in Throat: Persistent inflammation can lead to a sensation of a lump in the throat.
Symptoms are typically worse after consuming trigger foods, lying down, or eating late at night. If you experience severe chest pain, persistent vomiting, or difficulty swallowing, it’s important to visit an ER near me for immediate evaluation and care.
What Causes an Acid Reflux?
Several factors contribute to the development of acid reflux, primarily by weakening the LES or increasing abdominal pressure.
- Weak LES Muscle: The most common cause; allows acid to flow back into the esophagus.
- Certain Foods and Beverages: Spicy foods, fried meals, chocolate, caffeine, citrus fruits, carbonated drinks, and alcohol.
- Overeating: Large portions increase pressure inside the stomach, promoting reflux.
- Obesity and Abdominal Pressure: Extra weight pushes stomach contents upward, triggering acid reflux.
- Pregnancy: Hormonal changes and increased abdominal pressure elevate the risk of reflux.
- Hiatal Hernia: Part of the stomach slides through the diaphragm, interfering with LES function.
- Lifestyle Factors: Smoking and alcohol consumption relax the LES and contribute to reflux.
- Delayed Gastric Emptying: Slow digestion increases the likelihood of acid backing up into the esophagus.
How Long Does Acid Reflux Last?
The length and frequency of reflux episodes vary based on triggers and individual digestive health.
- Mild Reflux: May last a few minutes and often resolves naturally.
- After Large Meals: Symptoms may persist for hours due to slower digestion of heavy or fatty foods.
- Food-Specific Reflux: Certain foods can trigger longer-lasting episodes, particularly spicy, fatty, or acidic foods.
- Nighttime Reflux: Lying down extends exposure to acid, causing prolonged discomfort.
- Chronic Reflux or GERD: Frequent episodes several times a week may require medical evaluation and ongoing treatment.
How to Treat Acid Reflux
Treatment for acid reflux depends on the severity and frequency of symptoms. Most cases can be managed with lifestyle adjustments and medications, while persistent or severe symptoms may require professional care.
Lifestyle Changes
Small changes in daily habits can significantly improve acid reflux symptoms.
- Eat Smaller, More Frequent Meals: Reduces stomach pressure and prevents acid backflow.
- Avoid Trigger Foods and Beverages: Identify foods that worsen symptoms and reduce or eliminate them from your diet.
- Stay Upright After Eating: Waiting at least 2–3 hours before lying down reduces nighttime reflux.
- Maintain a Healthy Weight: Reduces abdominal pressure that can push stomach contents upward.
- Elevate the Head of Your Bed: Sleeping slightly upright can prevent nighttime acid reflux.
- Limit Alcohol and Caffeine: Both can relax the LES, increasing the likelihood of reflux.
- Quit Smoking: Smoking decreases LES tone and worsens symptoms.
- Wear Loose-Fitting Clothing: Tight belts or waistbands can exacerbate reflux by increasing abdominal pressure.
Over-the-Counter Medications for Acid Reflux
OTC medications provide quick relief for mild or occasional reflux symptoms.
- Antacids: Neutralize stomach acid to provide rapid symptom relief.
- H2 Blockers: Reduce the amount of acid produced in the stomach, offering longer-lasting relief.
- Proton Pump Inhibitors (PPIs): Strongly suppress acid production, ideal for chronic or frequent reflux.
- Guidelines for Safe Use: Follow instructions carefully to avoid complications from overuse.
Prescription Treatments for Chronic Acid Reflux
Persistent or severe acid reflux often requires professional medical intervention.
- Prescription Medications: Stronger H2 blockers or PPIs to control frequent reflux.
- Medical Testing: Endoscopy, pH monitoring, and esophageal manometry to assess damage and reflux severity.
- Prevent Long-Term Damage: Proper treatment prevents esophageal inflammation, strictures, or Barrett’s esophagus.
- Lifestyle Guidance: Combined with medical treatment, lifestyle changes enhance long-term outcomes.
Acid Reflux vs Heartburn vs GERD
Many people confuse these terms, but each has distinct meaning:
- Acid Reflux: Acid reflux is the actual process where stomach acid flows backward from the stomach into the esophagus. The esophagus is not designed to handle stomach acid, so when this happens, it can irritate or inflame the lining.
- Heartburn: Heartburn is the symptom, not the condition itself. It is the burning sensation in the chest or throat caused by acid reflux. When stomach acid irritates the esophagus, the nerve endings sense this irritation, producing the familiar burning feeling.
- GERD (Gastroesophageal Reflux Disease): GERD is a chronic or persistent form of acid reflux. It occurs when acid reflux happens frequently, typically more than two times per week, and starts to affect daily life or cause complications.
Emergency Situations Requiring Immediate Attention
While most reflux is manageable at home, certain signs demand urgent care:
- Severe Chest Pain: Can mimic heart attack symptoms; requires immediate evaluation.
- Difficulty Breathing: May indicate serious complications.
- Persistent Vomiting: Risk of dehydration and esophageal damage.
- Difficulty Swallowing: Could suggest esophageal narrowing or severe inflammation.
- Refractory Symptoms: Persistent discomfort despite lifestyle adjustments or OTC medications needs professional assessment.
Emergency Care for Acid Reflux
Patients experiencing acid reflux can receive expert evaluation and treatment at Texas emergency care center. Patients experiencing acid reflux can receive expert evaluation and treatment at Neighbors Emergency Center. Doctors assess symptoms, including heartburn, regurgitation, bloating, and throat irritation to determine the underlying causes and severity. Diagnostic procedures such as endoscopy and pH monitoring identify esophageal inflammation, irritation, or complications like Barrett’s esophagus. Personalized care plans include medications, diet modifications, and lifestyle changes to manage symptoms effectively. Continuous follow-up ensures long-term monitoring and prevents chronic damage. Emergency care is available for severe cases with chest pain, difficulty breathing, or persistent vomiting. Timely professional attention helps patients alleviate discomfort, improve digestion, and maintain overall health.
Frequently Asked Questions
Can you die from acid reflux in your sleep?
Acid reflux itself is rarely fatal, but severe cases of GERD can cause complications like esophageal damage or respiratory issues. Nighttime reflux increases the risk of choking, aspiration, or worsening asthma. Proper management and medical care can significantly reduce these risks.
Can acid reflux cause nausea?
Yes, acid reflux can irritate the stomach and esophagus, leading to nausea or an unsettled stomach. Symptoms often worsen after heavy or spicy meals. Persistent nausea should be evaluated by a healthcare provider.
Does acid reflux cause burping?
Yes, frequent burping can result from swallowed air and acid reflux. It often occurs after eating or drinking quickly, carbonated beverages, or trigger foods. Managing eating habits and avoiding certain foods can reduce excessive burping.


