It can feel overwhelming when you or someone you care about is diagnosed with diabetes, especially when trying to understand what it actually means. Diabetes is a chronic condition that affects how the body regulates blood sugar (glucose) using insulin. When this system is disrupted, glucose builds up in the blood and can lead to serious long-term health complications. Although often spoken of as one condition, diabetes mainly includes Type 1 and Type 2 diabetes, which are very different in how they develop and are managed.
Understanding the difference between Type 1 and Type 2 diabetes is important for early detection, proper treatment, and recognizing when symptoms require urgent medical attention, such as visiting an emergency room for diabetes care like an ER in Pearland.
What Is Type 1 Diabetes?
Type 1 diabetes is an autoimmune condition where the immune system destroys insulin-producing cells in the pancreas. This leads to little or no insulin production, causing blood sugar levels to rise dangerously. It usually develops in children or young adults and requires lifelong insulin therapy.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIH), Type 1 diabetes accounts for about 5–10% of all diabetes cases.
Type 1 Diabetes Symptoms That Should Never Be Ignored
- Excessive thirst: Constant dehydration caused by high blood sugar pulling fluids from tissues.
- Frequent urination: The body removes excess glucose through urine, increasing fluid loss.
- Sudden weight loss: Fat and muscle are used for energy due to lack of insulin.
- Extreme fatigue: Cells cannot access glucose, leading to weakness and exhaustion.
- Blurred vision: Fluid changes affect the eyes’ ability to focus properly.
What Is Type 2 Diabetes?
Type 2 diabetes is a long-term metabolic condition where the body becomes resistant to insulin or does not produce enough of it. This results in persistently high blood sugar levels that can damage organs such as the heart, kidneys, eyes, and nerves over time. It usually develops gradually and is strongly linked to lifestyle and genetic factors.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIH), Type 2 diabetes accounts for about 90–95% of all diabetes cases.
Type 2 Diabetes Symptoms That Are Dangerous
- Frequent urination: Kidneys work harder to remove excess sugar from the body.
- Extreme thirst: Ongoing dehydration leads to constant need for fluids.
- Unexplained weight loss: The body breaks down fat and muscle for energy.
- Blurred vision: High glucose levels affect fluid balance in the eyes.
- Slow healing wounds: Poor circulation delays recovery and increases infection risk.
If these symptoms worsen, seek urgent care near me immediately.
What Is the Difference Between Type 1 and Type 2 Diabetes?
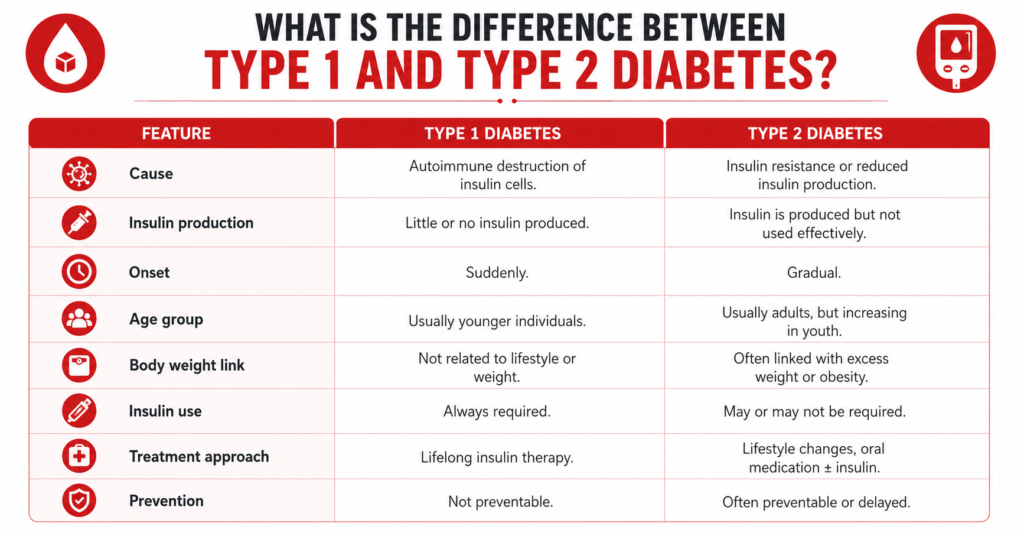
| Feature | Type 1 Diabetes | Type 2 Diabetes |
| Cause | Autoimmune destruction of insulin cells. | Insulin resistance or reduced insulin production. |
| Insulin production | Little or no insulin produced. | Insulin is produced but not used effectively. |
| Onset | Suddenly. | Gradual. |
| Age group | Usually younger individuals. | Usually adults, but increasing in youth. |
| Body weight link | Not related to lifestyle or weight. | Often linked with excess weight or obesity. |
| Insulin use | Always required. | May or may not be required. |
| Treatment approach | Lifelong insulin therapy. | Lifestyle changes, oral medication ± insulin. |
| Prevention | Not preventable. | Often preventable or delayed. |
Also Read: Is Diabetes Genetic?
What Causes Type 1 and Type 2 Diabetes?
Diabetes develops due to different biological and lifestyle-related factors depending on the type. While Type 1 diabetes is mainly driven by immune system dysfunction, Type 2 diabetes is more commonly linked to how the body responds to insulin over time. Understanding these causes helps in recognizing risk factors and taking early preventive steps where possible.
Type 1 Diabetes Causes
- Autoimmune reaction: The immune system mistakenly attacks insulin-producing cells in the pancreas, leading to little or no insulin production.
- Genetic factors: Family history can increase the likelihood of developing Type 1 diabetes, but it is not the only cause.
Type 2 Diabetes Causes
- Insulin resistance: The body’s cells do not respond properly to insulin, causing glucose buildup in the blood.
- Excess body weight: Fat accumulation, especially around the abdomen, reduces insulin effectiveness.
- Lifestyle factors: Poor diet, lack of exercise, and sedentary habits significantly increase the risk over time.
If you or a loved one experience symptoms, don’t delay seeking care. Visit the emergency room for diabetes management immediately.
Is Type 1 or Type 2 Diabetes Worse?
Neither type is worse, but both can become serious without proper management. Type 1 requires immediate insulin therapy because the body produces none, while Type 2 may develop silently and cause long-term damage if untreated.
- Type 1 diabetes is more immediately life-dependent due to lack of insulin.
- Type 2 diabetes may remain undetected for years and lead to complications like heart, kidney, and nerve damage.
Can Type 1 Turn Into Type 2 Diabetes?
No. Type 1 and Type 2 diabetes are completely different conditions. However, people with Type 1 may develop insulin resistance over time, sometimes called “double diabetes,” but one does not convert into the other. Both conditions still require careful long-term management to prevent complications affecting multiple organs. If needed, seek an emergency room near me for urgent medical care.
When to Go to the ER for Diabetes
Diabetes can become a medical emergency when blood sugar levels become extremely high or dangerously low. In these situations, the body may show warning signs like confusion, vomiting, or loss of consciousness that require immediate care. Delaying treatment can lead to serious complications such as diabetic coma or organ damage.
Type 1 Diabetes
- Diabetic ketoacidosis (DKA): Symptoms like vomiting, fruity breath, rapid breathing, or severe weakness require urgent ER care.
- Severe low blood sugar: Seizures, fainting, or inability to wake up need immediate treatment.
- Loss of consciousness: Sudden unresponsiveness is a life-threatening emergency.
Type 2 Diabetes
- Severe high blood sugar: Extreme thirst, dehydration, and confusion may signal a hyperglycemic crisis.
- Persistent vomiting: Inability to keep fluids down can quickly lead to dangerous dehydration.
- Confusion or drowsiness: High glucose levels may affect brain function and require urgent care.
Treatment for Type 1 and Type 2 Diabetes
Diabetes treatment focuses on keeping blood sugar stable and preventing long-term complications. It usually involves a combination of medication, lifestyle changes, and regular monitoring. Proper management helps reduce risks to the heart, kidneys, nerves, and overall health.
Type 1 Diabetes
- Insulin therapy: Lifelong insulin is required to replace what the body cannot produce. This includes injections or insulin pumps prescribed by the doctor.
- Blood sugar monitoring: Frequent glucose checks help maintain stable levels and prevent emergencies.
- Carbohydrate management: Balanced meals help match insulin doses with glucose intake for better control.
- Emergency glucose treatment: Fast-acting glucose is used to quickly treat dangerously low blood sugar episodes.
Type 2 Diabetes
- Oral medications: Medicines like metformin help improve insulin sensitivity and lower glucose levels prescribed by the doctor.
- Insulin therapy (if needed): Used when oral medications are not enough to control blood sugar prescribed by the doctor.
- Dietary changes: Reducing sugar, refined carbs, and eating fiber-rich foods helps stabilize blood sugar.
- Physical activity: Regular exercise improves insulin use and supports weight control.
- Weight management: Losing excess weight improves insulin response and reduces complications.
- Hydration and lifestyle habits: Drinking enough water and maintaining healthy routines support overall blood sugar control.
If you need urgent or ongoing care, search for diabetes treatment near me for timely medical support.
Diabetes Care at Texas Emergency Care Center
Living with diabetes requires ongoing attention, especially when symptoms become severe or unpredictable. Understanding the Difference Between Type 1 and Type 2 Diabetes helps with awareness, but emergency care is essential during unstable blood sugar events.
At Texas Emergency Care Center, patients receive fast evaluation and treatment for diabetes-related emergencies, including high or low blood sugar, dehydration, and confusion. Prompt care helps reduce complications and supports safer recovery.
Key Takeaways
- Diabetes is a condition where the body cannot properly control blood sugar due to insulin problems. Diabetes
- Main types are Type 1 and Type 2 diabetes, with different causes and treatments.
- Type 1 is an autoimmune condition with little or no insulin production. Type 1 Diabetes
- Type 2 involves insulin resistance and usually develops over time. Type 2 Diabetes
- Type 1 always needs insulin, while Type 2 may be managed with lifestyle changes and medication.
- Symptoms like extreme thirst, fatigue, and frequent urination should not be ignored.
- Early diagnosis and treatment help prevent serious complications.
FAQs
What is diabetes?
Diabetes is a condition where blood sugar stays too high because the body doesn’t make or use insulin properly.
How many types of diabetes are there?
There are two main types: Type 1 and Type 2 diabetes. Type 1 Diabetes Type 2 Diabetes
Can type 2 diabetes be reversed?
It may be put into remission with weight loss, diet changes, and exercise, but it is not always permanently cured.
How to know if you have diabetes?
Common signs include thirst, frequent urination, fatigue, and blurred vision. A blood test is needed for confirmation.


